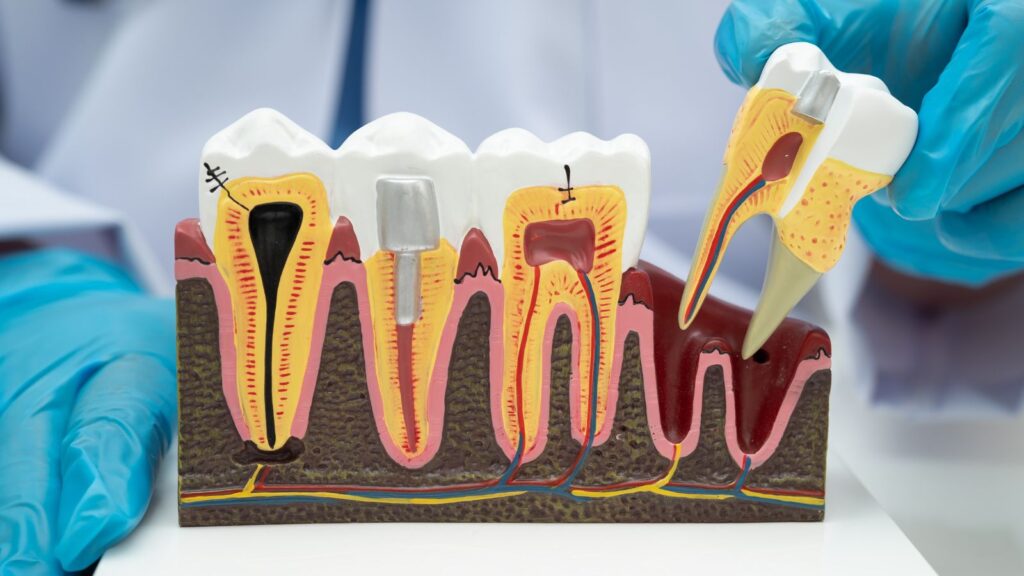
You can expect more predictable implant placement when you use digital planning and a custom surgical guide to translate virtual plans into the operating field. Digital workflows combine CBCT scans, intraoral scans, and CAD design to control implant position, angulation, and depth, reducing guesswork and improving prosthetic outcomes.
This article will show how the technology links virtual treatment planning to clinical reality, how that improves precision and healing, and what this means during surgery and for your long-term restoration. Learn practical advantages and what to expect during clinical implementation so you can make informed choices about guided implant care with Imagine Your Smile Dental Implant Center in Woodbury.
Digital Planning in Guided Implant Surgery
Digital planning centers on accurate 3D imaging, precise virtual implant positioning, and fabrication of surgical guides that transfer the plan to the mouth. You will use CBCT data, intraoral scans, and planning software to map bone anatomy, prosthetic needs, and surgical constraints before you touch the patient.
Role of 3D Imaging and Cone Beam CT
CBCT provides volumetric bone data you need for safe implant placement: bone height, width, and proximity to vital structures (sinus, nerve canal). Voxel size, field of view, and exposure settings affect image resolution, so choose parameters that balance diagnostic detail and radiation dose.
Use CBCT to measure cortical thickness and cancellous density when planning implant diameter and length. Combine CBCT with soft-tissue or intraoral scans to visualize emergence profile and gingival margins for prosthetic-driven placement. Recognize common artifacts—metal restorations or motion—so you verify anatomy clinically and with perioperative checks.
Digital Workflow for Implant Placement
Start by acquiring a CBCT and an intraoral scan or a lab-scanned model. Import both data sets into planning software (e.g., coDiagnostiX, SimPlant, NobelClinician) and register them using fiducial markers or surface-matching algorithms.
Plan implants prosthetically: position fixtures relative to planned crowns, check angulation, and simulate bone engagement. Review virtual osteotomy depth, drill sequence, and planned torque limits. Export the finalized plan as an STL or guide file for fabrication, and document measurements and surgical notes for intraoperative reference.
Integration With Surgical Guides
Surgical guides translate the virtual plan into controlled drill paths. You will choose between fully guided (pilot and sequential guided drilling plus guided implant insertion), pilot-only, or navigation-assisted approaches based on case complexity and instrumentation.
Verify guide fit on the model and in the mouth; rigid seating and index features reduce positional error. Confirm sleeve heights and drilling depths match the plan. Remember that guide accuracy depends on the entire chain—imaging quality, registration, software planning, and guide manufacturing—so validate each step before surgery.
Enhancing Precision and Outcomes
Digital planning and guidance tighten control over implant location, depth, and angulation while improving communication with the lab and surgical team. That control reduces guesswork, aligns the final prosthetic with anatomy, and shortens operative time.
Accuracy of Implant Positioning
You achieve submillimeter placement consistency by merging CBCT data with intraoral scans and planning implant position relative to adjacent teeth and prosthetic contours. Software lets you set depth stops and angulation limits, then translate that plan into a physical guide or navigation trajectory.
Clinical accuracy depends on factors you can control: scan quality, correct registration between datasets, guide fit, and surgical technique. Rigid, well-seated guides and verification of guide seating before osteotomy minimize deviation. Expect smaller horizontal and angular errors versus freehand placement in peer-reviewed reports, particularly for fully guided, tooth-supported guides.
Predictability of Surgical Results
You reduce variability in outcomes by standardizing the workflow from planning to placement. The digital plan documents implant diameter, length, and 3D position, so the team and lab share the same target for immediate or delayed loading.
Predictability improves for complex cases—narrow ridges, esthetic zones, or angled anatomy—because you can simulate prosthetic space and bone engagement before cutting. When you follow the plan precisely, prosthetic components fit with fewer adjustments and chairside time drops, which lowers the risk of restorative complications.
Reduction of Complications
You lower risk of critical complications—nerve injury, sinus penetration, and improper emergence profile—through preoperative 3D assessment and virtual avoidance of vital anatomy. The plan highlights safe zones and required bone augmentation before entering the OR.
Guides and navigation also reduce soft-tissue trauma by enabling flapless, minimally invasive approaches when bone and prosthetic planning allow. Fewer intraoperative surprises translate to less bleeding, reduced postoperative pain, and faster healing, provided you verify guide fit and maintain sterile, precise surgical technique.
Clinical Implementation and Patient Benefits
Digital planning and guided surgery change how you experience implant care, lowering surgical unpredictability and streamlining steps from diagnosis to prosthesis delivery. These tools affect comfort, case selection, and chair time in measurable ways.
Improved Patient Experience
Guided surgery reduces the need for large flaps and extensive tissue manipulation, so you typically face less postoperative pain and swelling. When clinicians use a surgical guide for depth and angulation control, they can perform more flapless or minimally invasive procedures, which shortens recovery and often allows earlier prosthetic function.
Clear visualizations from CBCT and intraoral scans improve communication about expected outcomes. You can review the planned implant position and prosthetic result before surgery, which helps set realistic expectations. Predictable placement also lowers the chance of unexpected additional procedures such as bone grafting or re-entry.
Case Selection and Suitability
You will benefit most when clinicians match the guided workflow to case complexity. Guided surgery suits single-tooth restorations, partially edentulous spans, and full-arch cases, especially when limited bone volume or proximity to vital anatomy exists. Use it when precise angulation is necessary for screw-retained prostheses or when immediate provisionalization is planned.
Contraindications include severe trismus, unstable soft tissues, or when intraoral landmarks cannot be captured reliably. Also consider patient factors—poor oral hygiene, uncontrolled systemic disease, or inability to tolerate longer preoperative imaging can make guided approaches less appropriate. Clinicians should evaluate bone quality, prosthetic demands, and access before committing to a fully guided protocol.
Time Efficiency in Treatment
Digital workflows compress several clinical steps into fewer visits. A single appointment can capture CBCT and digital impressions, enabling planning and guide fabrication without repeated physical impressions. This reduces patient visits and cumulative chair time.
Intraoperatively, guided templates streamline osteotomy sequence and implant insertion, cutting surgical time for experienced teams. Laboratory and restorative steps also tighten: CAD/CAM fabrication of provisionals and final restorations often overlaps with surgical planning, so you receive provisional restorations sooner. Track turnarounds and lab coordination to ensure scheduled efficiencies materialize in your treatment.