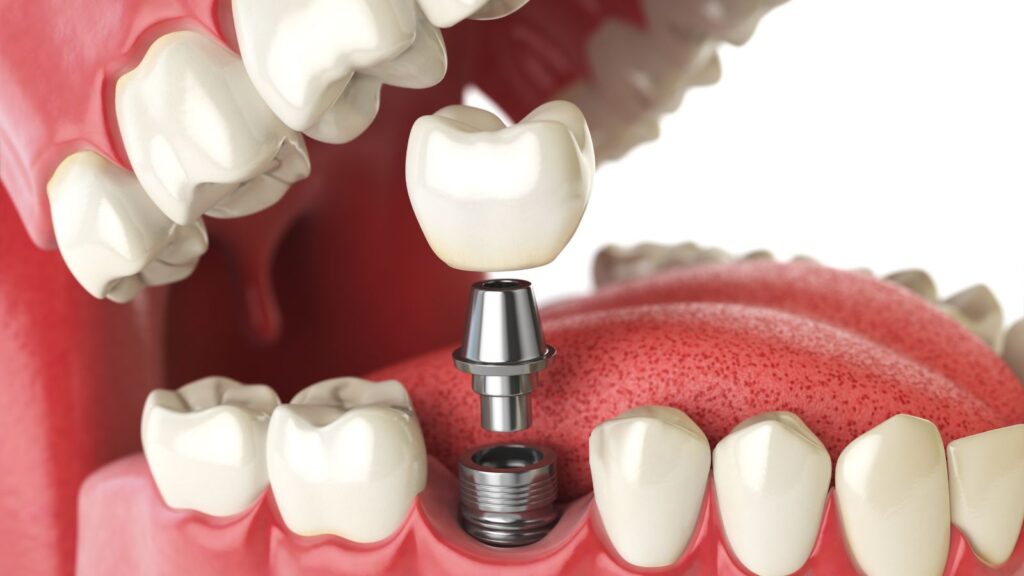
If your upper jaw lacks the bone needed for traditional implants, zygomatic implants let you get stable, long-lasting teeth by anchoring into the dense cheekbone instead of the failing maxilla. This approach avoids lengthy bone grafting and can restore function and appearance for patients who otherwise had few options.
You will learn how severe maxillary bone loss develops, what makes zygomatic implants different, how clinicians plan and place them, and what outcomes and risks to expect. The rest of the article breaks down eligibility, the surgical pathway, recovery expectations, and the realistic benefits you can expect over the long term, especially if you are exploring dental implants in Melissa TX
Understanding Severe Upper Jaw Bone Loss
Severe upper jaw bone loss can change how your face looks, make dentures unstable, and limit options for fixed teeth. You’ll learn why the maxilla shrinks, how that affects chewing, speech, and facial support, and why standard implants often fail in these cases.
Causes of Maxillary Bone Loss
Bone in the upper jaw (maxilla) resorbs when it no longer receives normal forces from teeth or roots. Long-term tooth loss is the most common cause; within months to years the ridge flattens and height reduces.
Chronic periodontal (gum) disease and repeated infections accelerate bone destruction by breaking down the supporting bone around remaining teeth. Trauma and surgical removal of tumors or cysts can remove large volumes of bone directly.
Systemic conditions—uncontrolled diabetes, osteoporosis, and long-term corticosteroid use—also impair bone maintenance and reduce healing capacity. Radiation therapy to the head and neck further compromises local bone health and increases risk of implant failure.
Impact on Oral Health
Severe maxillary bone loss undermines denture fit and stability, causing sore spots, slippage, and difficulty chewing firmer foods. You may notice reduced bite force and altered speech, especially with missing anterior teeth that affect lip support and phonetics.
Facial aesthetics change: loss of maxillary height causes midface flattening and increased nasolabial fold prominence, which can make the lower face appear more prognathic. Nutritional intake can suffer when chewing becomes limited, increasing risks of weight loss or dietary compromises.
Bone loss also complicates future dental work by reducing available bone volume and altering sinus anatomy, which can increase risks during surgery.
Challenges in Standard Dental Implant Placement
Standard implants rely on adequate vertical and horizontal bone in the alveolar ridge for primary stability and long-term integration. With severe maxillary atrophy you may lack the bone height above the maxillary sinus and the thickness needed to place conventional implants safely.
Common solutions—bone grafting and sinus lifts—require multiple surgeries and months of healing; they may still fail in patients with poor healing potential or irradiated bone. You face higher risk of sinus perforation, implant instability, and prolonged treatment timelines when using standard implant approaches.
These constraints often lead clinicians to consider alternative anchorage sites or implant designs that bypass the deficient alveolar bone.
What Are Zygomatic Implants?
Zygomatic implants are long titanium posts anchored in the cheekbone to support fixed dental restorations when your upper jaw lacks enough bone for standard implants. They let you avoid multi-stage bone grafting in many cases and can often support a full-arch prosthesis.
Unique Features of Zygomatic Implants
Zygomatic implants are 30–52 mm long—much longer than conventional implants—so they bypass the maxillary bone and engage the dense zygomatic (cheek) bone for primary stability. Their length and angulation allow surgeons to achieve strong fixation even when the posterior maxilla has severe atrophy or sinus pneumatization.
Placement typically requires a specialist (oral surgeon or maxillofacial surgeon) familiar with advanced anatomy and imaging-guided planning. Because the implant anchors in cortical zygoma bone, you often get immediate or early loading options, meaning a fixed prosthesis can be attached the same day or within days in selected cases.
Risks differ from standard implants: possible sinus involvement, altered cheek sensation, or soft-tissue management issues. Preoperative CT scans and careful surgical planning reduce those risks and help determine exact implant trajectory.
Comparison With Traditional Dental Implants
Traditional implants anchor into the maxillary or mandibular alveolar bone and commonly measure 8–15 mm. They require sufficient vertical and horizontal bone volume; otherwise you must have bone grafting or sinus lifts before implant placement.
Zygomatic implants avoid those grafting procedures by using the zygomatic bone as the anchor. That shortens overall treatment time and reduces graft-related morbidity. However, the surgery is more complex and has different complication profiles than conventional implants.
Many treatment plans use a hybrid approach: two zygomatic implants in the posterior plus two or more conventional anterior implants to create a stable full-arch support. This combination balances surgical complexity, prosthetic load distribution, and long-term function.
Who Is a Candidate for Zygomatic Implants
You may qualify if you have severe posterior maxillary bone loss from long-term tooth loss, periodontal disease, trauma, or multiple failed implants, and if bone grafting is impractical or undesirable. Candidates often seek a fixed full-arch solution rather than removable dentures.
Your surgeon will assess candidacy using a cone-beam CT to evaluate zygomatic bone quality, sinus anatomy, and prosthetic space. Medical history, smoking status, and any chronic conditions (e.g., uncontrolled diabetes) also affect eligibility.
If you want to avoid multiple grafting surgeries and accept a more advanced surgical procedure, zygomatic implants can be a viable option. Your implant team will outline risks, alternatives, and a rehabilitation timeline before proceeding.
Treatment Approach With Zygomatic Implants
This approach replaces missing upper teeth by anchoring long implants into your zygomatic (cheek) bone to bypass deficient maxillary bone. It involves careful imaging and planning, a surgical placement that may allow immediate provisional teeth, and a predictable recovery pathway with staged follow-up.
Pre-Surgical Assessment
You will receive a CBCT scan to map your maxilla, zygoma, sinus anatomy, and nerve locations precisely. The 3D data lets your surgeon measure bone thickness, choose implant length and trajectory, and plan whether one or two zygomatic implants per side are needed.
Medical history review is mandatory. Your surgeon assesses smoking status, uncontrolled diabetes, osteoporosis treatment (e.g., bisphosphonates), and prior sinus disease because these affect healing and risk. Expect blood tests or medical clearance if you have cardiac or bleeding conditions.
Treatment planning often uses surgical guides or virtual planning software. You and your clinician will discuss immediate-loading options (fixed provisional teeth within 24–48 hours) versus delayed loading based on primary stability and soft-tissue concerns.
Procedure Overview
The operation typically occurs under general anesthesia or IV sedation for comfort. Your surgeon exposes the alveolar crest and creates an osteotomy angled posteriorly and superiorly toward the zygomatic bone.
Zygomatic implants—considerably longer than standard implants—are threaded into the zygoma to achieve dense cortical engagement. Your team monitors implant torque; primary stability above protocol thresholds supports immediate provisionalization.
Soft-tissue management is critical. The surgeon contours gingiva, manages sinus membranes if entered, and places multi-unit abutments or prosthetic components. If immediate fixed teeth are planned, a lab or CAD/CAM system attaches a provisional bridge the same day or within 48 hours.
Recovery Timeline
First 48–72 hours focus on pain control, swelling reduction, and infection prevention. You will receive analgesics, antibiotics, and sinus-care instructions; cold packs and head elevation help swelling.
First two weeks involve suture removal (if non-resorbable used) and limited chewing on the treated side. You should avoid heavy exertion, nose-blowing, and activities that raise sinus pressure to reduce complication risk.
By 6–12 weeks the implant–bone interface matures; if delayed loading was chosen, definitive prostheses are often placed then. Full soft-tissue healing and prosthetic adjustments typically conclude by 3–6 months, with routine maintenance visits scheduled every 3–6 months thereafter.
Benefits and Long-Term Outcomes
Zygomatic implants can restore fixed upper teeth for patients with severe maxillary bone loss, often without lengthy grafting. They typically shorten treatment time, provide stable support, and carry documented long-term survival rates in experienced hands.
Advantages Over Bone Grafting
Zygomatic implants anchor in the dense zygomatic (cheek) bone instead of relying on an atrophied maxilla. That lets you avoid or minimize sinus lifts and large autografts, reducing surgical stages and overall treatment time.
You can often receive a fixed provisional prosthesis within days of surgery rather than waiting 6–12 months for graft consolidation. Clinically, this translates to fewer surgeries, lower cumulative operative risk, and often lower total cost.
Key practical advantages:
- Immediate function for chewing and speech in many cases.
- Use of longer implants with strong cortical engagement for primary stability.
- Access to implant therapy for patients previously told they were unsuitable for conventional implants.
Patient Success Stories
Many patients report rapid return to normal eating and improved confidence after zygomatic implant rehabilitation. Case series and systematic reviews show high implant survival—often above 90% at 5–10 years—when placed by surgeons experienced in the technique.
You should expect follow-up care that includes prosthesis maintenance, periodic imaging, and oral hygiene monitoring. Patient-reported outcomes commonly note improved comfort, better mastication, and higher satisfaction compared with removable dentures.
Realistic expectations:
- Maintenance needs (screw checks, hygiene) are ongoing.
- Success correlates strongly with surgical expertise and prosthetic planning.
- Past sinus disease or smoking can influence individual results.
Potential Risks and Considerations
Zygomatic implant placement is more complex than standard implant surgery and carries specific risks. These include sinusitis, oroantral communication, sensory changes, and, rarely, implant failure or malposition requiring revision.
You should have comprehensive imaging (CBCT) and a clear prosthetic plan before surgery. Choosing a clinician with zygomatic experience reduces complication rates. Preexisting sinus conditions, smoking, uncontrolled systemic disease, and poor oral hygiene increase your risk and may require treatment or modification before proceeding.
Practical risk-management steps:
- Preoperative CBCT and virtual planning.
- Antibiotic and sinus management protocols when indicated.
- Regular postoperative reviews and timely prosthetic maintenance.