If you want more stability, comfort, and chewing function than traditional dentures without the cost and surgery of full fixed implants, implant overdentures give you that middle ground by snapping onto two or more implants for secure support while remaining removable for cleaning.
You’ll explore what implant overdentures are, how they compare to full dentures and full-arch implants, what the treatment involves, and what to expect for maintenance, longevity, and cost—so you can decide if this hybrid option fits your goals and budget.
Start here to learn the practical trade-offs—stability versus invasiveness, cost versus permanence—and how implant overdentures may deliver the best balance for your lifestyle and oral health.
What Are Implant Overdentures?
Implant overdentures anchor removable dentures to dental implants to improve stability, chewing, and speech. They combine implant fixtures in the jaw with a removable prosthesis that you can take out for cleaning.
Definition and Key Components
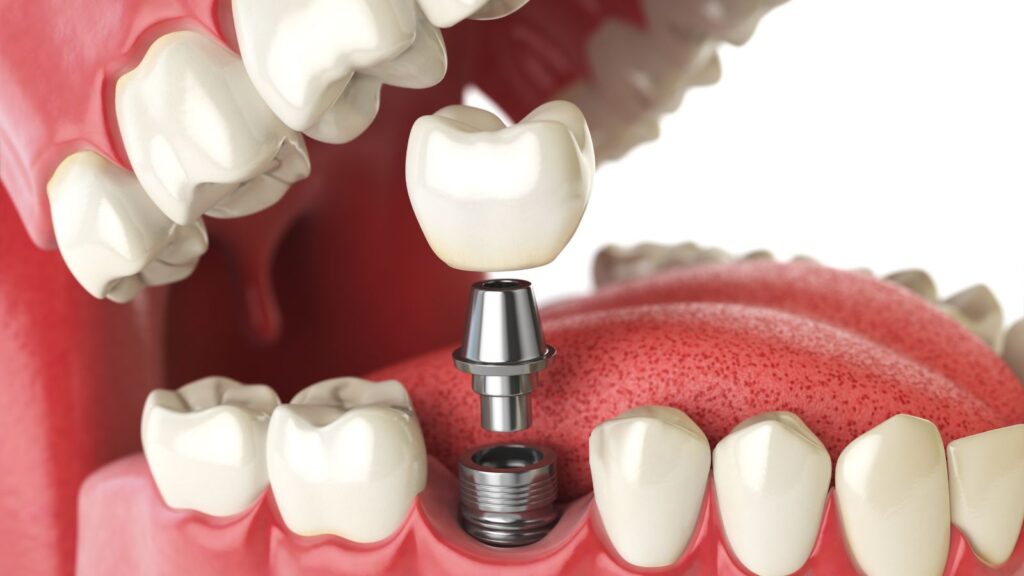
An implant overdenture is a removable denture that attaches to two or more dental implants placed in your jaw. The implants are small titanium posts surgically placed into bone; they osseointegrate (bond) with bone to provide secure anchorage.
Key components include:
- Implants: typically 2–4 per arch for overdentures, chosen based on bone quality and arch stability.
- Attachments: housings, ball attachments, bars, or locator systems that connect the denture to the implants.
- Denture base and teeth: acrylic or hybrid base with replacement teeth designed to sit on the soft tissues and engage the attachments.
You retain the ability to remove the prosthesis daily, and most designs rely on both implant support and soft-tissue contact to share chewing forces.
How Implant Overdentures Work
You secure the denture by snapping or clipping attachment elements on the denture into the implant-supported counterparts. The attachments provide retention and limit denture movement during function, which reduces sore spots and improves bite force.
Most overdentures are soft-tissue supported: the denture base still rests on your gums while implants carry a portion of the occlusal load. This shared load reduces pressure on the mucosa and transfers stabilization to the implants, improving comfort and chewing efficiency compared with conventional dentures.
You remove the prosthesis for hygiene; the attachments are replaceable components that may need periodic maintenance. Implant planning considers implant number, position, and attachment type to optimize retention and long-term function.
Types of Implant Overdentures
Common types classify by attachment and by how many implants support them.
By attachment:
- Locator attachments: low-profile, forgiving for minor misalignment; widely used.
- Ball-and-socket: simple ball studs with replaceable caps in the denture.
- Bar-retained: a rigid metal bar splints implants together; the denture clips onto the bar for increased stability.
By implant count:
- Two-implant overdenture: standard for a lower arch; cost-effective and common.
- Three- or four-implant overdenture: offers greater stability and is often used for upper arches or when bone conditions permit.
Choose attachment and implant number based on your jaw anatomy, functional needs, and budget. Clinicians balance retention, ease of hygiene, maintenance frequency, and long-term bone support when recommending a type.
Comparing Implant Overdentures, Full Dentures, and Full Implants
You’ll see differences in stability, cost, maintenance, and surgical complexity. Each option changes how you eat, speak, and care for your mouth.
Benefits Over Traditional Dentures
Implant overdentures attach to two to four implants, which prevents the slipping common with full removable dentures. That stability improves chewing efficiency and reduces sore spots on the gums.
You’ll regain more bite force than with conventional dentures, often allowing firmer foods without worry. Overdentures also preserve jawbone height better than dentures because the implants transmit some chewing forces to the bone.
Maintenance is straightforward: remove and clean the prosthesis daily and visit your dentist for periodic retainer or attachment checks. Costs sit between traditional dentures and full-arch implant bridges, giving a strong functional upgrade for a moderate investment.
Key Differences from Full Implant Restorations
Full implant restorations (fixed implant bridges) typically use 6–8 implants per arch and stay permanently in place. You won’t remove them, and they feel most like natural teeth in terms of stability and bite force.
Overdentures use fewer implants and are removable, so they require less surgical time, lower upfront cost, and often simpler bone requirements. However, overdentures transfer less chewing force to the jaw than fixed bridges and may need attachment replacement every few years.
If you want the highest long-term function and are willing to undergo more surgery and expense, fixed implants are the superior choice. If you prioritize lower cost, easier repairs, and still significant improvement over dentures, overdentures are the pragmatic middle ground.
Candidacy and Suitability
You’re a good candidate for implant overdentures if you have moderate jawbone volume, want improved stability, and prefer a removable appliance. Implant overdentures work well when full fixed implants are too costly or bone grafting is undesired.
Full dentures suit patients with limited budgets or medical conditions that preclude implant surgery. Fixed implant restorations suit healthier patients with adequate bone, higher budget, and desire for permanently anchored teeth.
Your dentist will evaluate bone density, medical history, oral hygiene habits, and budget to recommend the right option. Expect X-rays or CBCT scans, a treatment timeline, and discussion of maintenance demands before deciding.
Treatment Process for Implant Overdentures
You will move from evaluation and planning through implant surgery to prosthesis fitting and follow-up care. Each step focuses on restoring stable chewing, comfortable fit, and maintainable hygiene.
Initial Consultation and Planning
During your first visit the clinician reviews medical history, medications, and oral health risks that affect implant success. Expect a clinical exam, panoramic and/or CBCT imaging to measure bone volume, assess nerve and sinus positions, and plan implant locations.
Your dentist will discuss options—number of implants (commonly 2–4 in the mandible), attachment types (ball, locator, bar), and whether immediate loading is possible. They will create a treatment plan with timelines, cost estimates, and consent forms that outline risks and alternatives.
If bone augmentation or extractions are needed, the plan will include those procedures and additional healing time. You should receive preoperative instructions covering antibiotics, smoking cessation, and fasting if sedation is planned.
Implant Placement Procedure
On the day of surgery you will receive local anesthesia, sedation, or general anesthesia as indicated by the treatment plan. The surgeon exposes the bone, positions pilot holes using the surgical guide from your plan, then places titanium implants at predetermined depths and angles.
Typical mandibular overdenture treatment uses two implants; clinicians often place four for a bar-supported overdenture or to increase stability. If primary stability is high, temporary overdentures can be attached immediately; otherwise the implants remain covered for osseointegration.
Sutures close the sites and postoperative instructions address pain control, diet, oral hygiene, and signs of complications. You will receive a prescription for analgesics and sometimes antibiotics, plus written care guidance for the first 7–14 days.
Fitting and Adjustments
After osseointegration (usually 2–4 months), you return for prosthetic steps: connection of abutments or attachments, impression taking, and trial of the denture base and teeth arrangement. The clinician checks vertical dimension, occlusion, phonetics, and esthetics during try-ins.
Once the final overdenture is processed, your provider adjusts attachment retention and soft-tissue contacts chairside. They instruct you how to attach and remove the prosthesis, clean attachment components, and replace worn nylon inserts or clips when retention weakens.
Plan follow-up visits at 1–2 weeks, then at 3–6 months, and annually. At these visits the clinician evaluates tissue health, attachment wear, occlusion, and peri-implant bone levels via radiographs.
Expected Recovery Timeline
Immediate postoperative days focus on pain control, swelling reduction, and a soft-food diet. Most patients resume light activities within 48–72 hours; avoid strenuous exercise and hard foods for the first 1–2 weeks.
Osseointegration for mandibular implants typically takes 8–12 weeks; maxillary implants may require longer if bone quality is lower. If you receive immediate-load overdentures, expect more frequent early adjustments to address soreness and retention issues.
Long-term recovery includes adaptation to the prosthesis—learning removal, cleaning, and speech adjustments—which commonly stabilizes over 2–6 weeks. Maintain regular hygiene and recall visits to detect attachment wear or peri-implant changes early.
Maintenance, Longevity, and Cost Considerations
Expect routine daily care, periodic professional maintenance, and upfront costs that vary by implant number and prosthesis type. Your choices about attachments, materials, and follow-up visits determine both long-term function and total expense.
Daily Care and Hygiene Recommendations
Clean attachments and the prosthesis every day to prevent plaque, food buildup, and irritation. Remove removable overdentures at night when instructed, rinse them, and brush with a non-abrasive denture brush and mild soap or denture paste.
Care for implants and surrounding gums with a soft toothbrush and low-abrasive toothpaste twice daily. Use an interdental brush or soft-pick around implant abutments or locator housings to remove trapped debris. Consider a water flosser on low setting if manual access is difficult.
Inspect attachment components weekly for wear or loosening. Replace worn nylon inserts or replace maintenance parts per your clinician’s schedule—typically every 6–24 months—to maintain retention and avoid sudden failure.
Durability and Lifespan
Implant fixtures commonly show high survival rates when placed and restored properly; individual implants can last decades with good care. The overdenture prosthesis and attachment parts wear faster than implants and usually need periodic replacement.
Expect nylon inserts, O-rings, and locator components to require replacement every 6–24 months depending on chewing forces and hygiene. Acrylic denture bases may fracture or wear over 5–10 years; switching to a metal-reinforced bar can extend prosthesis life but raises costs.
Plan on regular maintenance visits—at least annually, often semiannually—for professional cleaning, occlusal checks, and component replacement. Promptly address looseness, sore spots, or unusual noises to prevent implant complications.
Cost Comparison and Investment Value
Two-implant overdentures generally cost less upfront than full-arch fixed implant bridges. Typical ranges for 2-implant overdentures are often lower than fixed solutions, with additional implants adding around $2,000–$4,000 each depending on location and clinician fees.
Factor recurring costs: periodic attachment replacements, prosthesis repairs, and maintenance visits. Higher initial investment in stronger materials or additional implants can reduce repair frequency and improve stability, potentially lowering long-term costs.
Use a simple checklist when comparing options:
- Upfront fees (surgery, implants, prosthesis)
- Recurring maintenance (inserts, relines, repairs)
- Expected replacement timeline (inserts vs. base vs. implants) Ask for an itemized estimate and a maintenance schedule from your provider to compare real lifetime costs for the choices you’re considering.